182 Rural Hospitals Closed.
Yesterday, Congress Was Finally Asking Why.
In 2010, Congress banned physician-owned hospitals. The data showed they had better outcomes at a lower cost. That’s exactly why they were banned.
2010: Congress bans new physician-owned hospitals.
2010-2025: Hospital systems consolidate without restriction.
2026: 182 rural hospitals have closed.
Today, the AMA finally tweets support for partial repeal.
50 years of monopoly protection.
One tweet doesn’t erase that.
But it’s a start.
IN TODAY’S ARTICLE:
The 2010 law that froze physician-owned hospitals in place while hospital systems consolidated without restriction
What the research actually shows about cost, quality, and outcomes at physician-owned facilities
Why the AHA is spending millions to keep the ban in place
What H.R. 2191 would change and who’s fighting it.
We will continue our AMA series on the morrow (I was reading Shakespeare with the kiddos).
Glossary at the bottom of today’s article.
THE BAN
In March 2010, Congress passed the Affordable Care Act.
Buried deep inside was Section 6001.
The provision banned new physician-owned hospitals from participating in Medicare. It froze existing physician-owned facilities in place. No new beds. No new operating rooms. No expansion.
The American Hospital Association lobbied hard for this provision. Their argument: physician owners would self-refer patients to their own facilities, cherry-pick the healthiest cases, and leave traditional hospitals with the sickest and poorest patients.
Members of Congress were paid off.
The ban passed.
Physician-owned hospitals, which had grown from 67 facilities in the early 2000s to roughly 250 by 2010, suddenly stopped growing.
Meanwhile, traditional hospital systems faced no such restrictions.
They consolidated. They merged. They acquired.
And 182 rural hospitals closed.
The people consolidating your market read this at 6am.
You're finding out at noon.
That gap is expensive.
Membership.
THE DATA THE AHA DOESN’T WANT YOU TO SEE
The AHA’s argument was simple: physician-owned hospitals are more expensive and lower quality.
The research says otherwise.
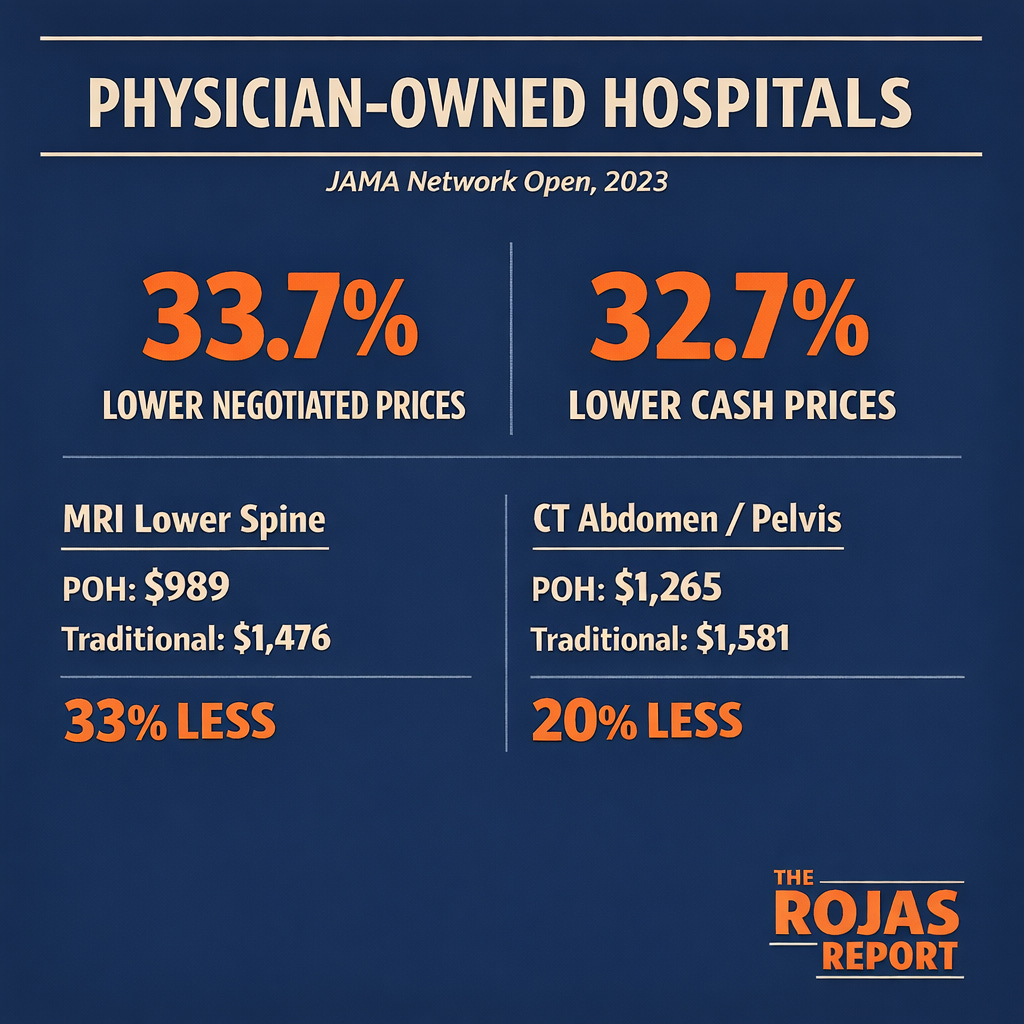
A 2023 study published in JAMA Network Open examined 156 physician-owned hospitals and 1,116 non-physician-owned facilities across 78 hospital referral regions.
The findings:
Median commercial negotiated prices were 33.7% lower at physician-owned hospitals.
Cash prices were 32.7% lower.
For an MRI of the lower spinal canal, physician-owned hospitals charged $989. Traditional hospitals charged 33% more.
For a CT scan of the abdomen and pelvis, the difference was 20%.
The researchers expected to find the opposite. They hypothesized that physician ownership would lead to higher prices.
The data proved them wrong.
Additional research in The Spine Journal found that physician-owned hospitals had lower complication rates and lower overall costs for lumbar fusions than non-physician-owned facilities.
A systematic review of 30 years of research concluded that physician-owned specialty hospitals offer higher-quality care at comparable or lower cost.
The cherry-picking argument? A BMJ study found that physician-owned hospitals were just as likely to treat Medicaid patients and patients from racial minority groups as traditional hospitals.
The AHA’s entire justification for the ban was based on predictions.
The predictions were wrong…