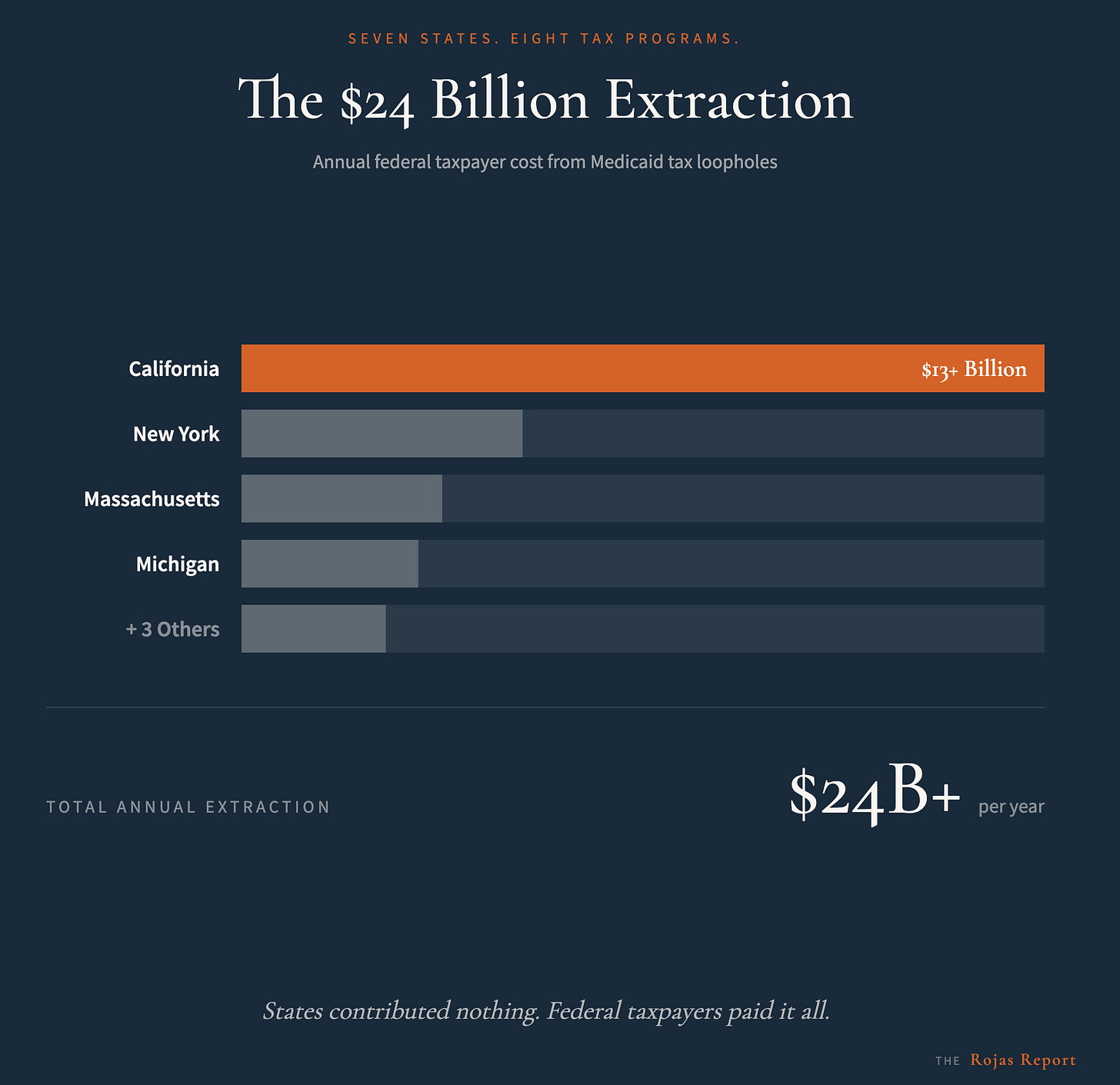
Seven States Ran a $24 Billion Scam on Federal Taxpayers. This Week, CMS Shut It Down.
California taxed Medicaid plans 157 times higher than commercial plans. Then reimbursed the insurers entirely with federal dollars. The state kept the difference. You paid for it.
States are required to pay their share of Medicaid expenses.
Seven states found a way to pay nothing.
They taxed Medicaid insurers at rates up to 157 times higher than commercial insurers. They then reimbursed those insurers in full with federal matching funds.
The insurers paid nothing net.
The states paid nothing net.
Federal taxpayers paid it all.
IN TODAY’S ARTICLE:
How states exploited a statistical test to impose 157x higher taxes on Medicaid business
California’s $13 billion extraction (out of $24 billion total)
The federal response: Public Law 119-21 and the January 29, 2026, final rule
The connection between state Medicaid gimmicks and your commercial premium increases
Glossary at the bottom of today’s article.
THE ANNOUNCEMENT
On January 29, 2026, CMS announced a final rule closing what it called a “massive Medicaid financing loophole.”
The agency didn’t mince words. CMS Administrator Dr. Mehmet Oz said states “relied on loopholes to offload their responsibilities onto federal taxpayers” and directed Medicaid spending to favored hospitals and health systems rather than to families who depend on the program.
The numbers back him up.
Seven states ran eight tax programs that extracted over $24 billion annually from federal taxpayers. California alone generated more than $13 billion through this mechanism.
The states paid nothing essentially.
THE MECHANISM
The scheme worked like this.
Federal law allows states to tax healthcare entities to help fund their share of Medicaid. The taxes must be “broad-based” and “uniform.” States can’t just tax Medicaid business at higher rates than non-Medicaid business.
Except they did.
California taxed Medicaid managed care organizations $274 per member per month. Commercial plans? $1.75 per member per month.
That’s a 157-to-1 ratio.
The federal regulations included a statistical test called the “B1/B2 test” to catch non-uniform taxes. States gamed the test. They imposed taxes so disproportionately weighted toward Medicaid business that the test became meaningless. The regulators built a lock. The states picked it.
Then came the second part of the scheme.
States collected the tax revenue. They used it as their “state share” to draw down federal matching funds. Federal matching rates range from 50% to 77%, depending on the state. So for every dollar of tax revenue, states could claim one to three additional federal dollars.
Then, states reimbursed the taxed entities in full with federal matching funds.
The insurers paid tax. Got it back. Net cost: zero.
The states collected tax.
Got federal match.
Paid back the insurers.
Kept the difference.
Net contribution: zero.
Federal taxpayers funded the entire scheme.